“This is your brain. This is drugs. This is your brain on drugs. Any questions?”
Simplicity is what made this 1980s-public service announcement—in which a man cracks an egg into a heated frying pan to illustrate the damage caused by drugs—compelling. One plus one equals two. If you do drugs, they ruin your life. Period.
Yet in reality, drug addiction is not that simple.
A quarter of a billion people use illicit drugs annually. This is despite the increased risk of overdose, which has gone up 33 percent in the United States over the last five years, according to the Centers for Disease Control and Prevention.
At the front end of increasing drug use is heroin, which is now the number-one killer among illegal drugs. Given its resurgence over the past decade, the old stigma of it being confined to inner cities, the poor, and minorities is fading. The highly addictive drug now grips rural towns and wealthier suburbs.
The story of an Ohio couple interviewed by The Columbus Dispatch shows heroin abuse’s impact. The 39-year-old man, who became hooked on painkillers after dislocating his shoulder, once dreamed of working in law enforcement. Instead, he became addicted to the drug after he discovered that the $10 to get high from heroin is more sustainable than paying $80 per pill for painkillers.
His girlfriend, who aspired to work in a veterinarian’s office, began her struggle with drug abuse after accepting an OxyContin pill from her boyfriend. Their four children were eventually taken by authorities and put up for adoption.
Twelve years or so into their addiction, the couple, now frail and haggard, spend their days scouring streets and rummaging dumpsters for soda cans and other recyclables to sell to support their habit. On a good day, they earn enough to split a dose of heroin the size of a watermelon seed.
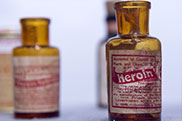
The beginning: Antique prescription heroin bottles are on display at the Drug Enforcement Agency Museum in Arlington, Virginia (Aug. 25, 2015).
“It just makes you feel more of what you are supposed to be,” the man explained in a video interview posted by the newspaper. “I know there is normal, but this makes you feel above and beyond normal. It makes you feel you can do way more than what you can.”
“It makes you feel like you are Superman…” he added.
This explains why the drug is so hard to kick—heroin rewires the brain and makes you feel invincible. Brad Lander, clinical director of addiction medicine at Ohio State University’s Wexner Medical Center, explained in a Columbus Dispatch article that heroin “changes the brain and the user’s reality.”
He described how heroin activates the brain’s release of adrenaline and endorphins—the body’s naturally occurring “opiate system” that normally provides energy and helps relieve pain when we get hurt. Once addicted, the brain thinks it needs heroin just to function.
“You need to have it, or you feel dysphoric, sad, anxious, depressed,” Dr. Lander continued. “Any pain you have is exaggerated.”
He likened an addict being denied heroin to a person starving to death.
“If you’re starving to death, you’ll take more risks with employment and relationships. You would steal more things if you were really starving to death. So [addicts] are doing things they never thought they would do.”
This depiction of hopeless dependence has replicated itself across America—from bustling streets in downtown Seattle, Washington, to quaint fishing towns in Massachusetts. As a result, those on the front lines are trying a new approach: Instead of focusing on stopping its usage, the fight has turned to minimizing the drug’s effects.
In short, in the modern war on heroin, authorities are beginning to lay down their weapons.
Making a Comeback
Introduced nearly 120 years ago for commercial use by the pharmaceutical company Bayer, heroin, which is derived from the opium poppy plant, was originally seen as a wonder drug. It quickly became a vital component of pain management, as chemicals in it suppressed pain receptors in the brain and spinal cord.
By 1924, however, it became illegal after doctors learned of its addictive qualities. Yet this did not stop a population suffering from chronic pain from wanting relief. This prompted the medical community to turn to less potent forms of the opioid to treat pain. As a result, illegal heroin mostly disappeared—other than for a brief stint in the 70s—and became overshadowed by other banned substances such as cocaine and marijuana.
Torn apart: A woman whose husband died of a heroin overdose holds her children in her bedroom in Plainville, Connecticut (March 6, 2016).
Fast forward 20 years. The early 1990s saw a rise in prescription opioid requests. According to the National Institute on Drug Abuse, prescriptions for hydrocodone (used in Vicodin) and oxycodone (used in Percocet) jumped from 44 million in 1991 to 73 million in 1996. The spike in demand resulted in the release of OxyContin, a concentrated form of oxycodone, that same year.
As opiate-based medications crept closer to the potency of heroin, pharmaceutical marketers were forced to address fears of addiction. Thus the creators of OxyContin went on a media blitz in 1998, sending promotional materials to doctors’ offices and placing product advertisements in medical journals. The ads touted the pill’s effectiveness against pain as well as the unlikelihood of chemical dependence.
In response, opioid prescriptions jumped 10 percent the following year. The makers of OxyContin raked in billions in sales and profits as doctors continued to hand out pills to those who they thought needed them.
Eventually it was discovered that people were using the pills to get high. And authorities later learned that the manufacturer of OxyContin misled regulators, doctors and patients about the drug’s risks of addiction and its potential for abuse.
Following a lawsuit and steep fine, the makers of OxyContin tweaked the formula, adding what they referred to as “abuse deterrents”—designed to make the pills more difficult to crush into powder, for example, so that they could not be snorted or injected.
Ironically, this move is what many point to as the true start of the heroin crisis. The modification had the unintended consequence of pushing those who were already addicted to the pain pills toward heroin. The illegal substance was cheaper ($10 per hit versus $60-100 per pill), easier to find, easier to use, and—most important to a craving addict—much more powerful.
Newfound Markets
The shift from painkillers to heroin across America has been a boon for drug cartels. Weary of stiff competition in major metropolitan areas such as New York City or Chicago, drug syndicates have set up shop in suburbs and small towns. Dealers know that a successful illegal drug ring thrives on access to certain elements, namely money, communication (e.g. cellphones), transportation and privacy for drug use. Suburbia and many rural towns offer an abundance of each.
Another benefit for cartels regarding small towns is the lack of adequate law enforcement. Most small unassuming areas have never experienced anything like the current heroin crisis—and are thus ill-equipped and ill-prepared to handle it.
“Out-of-town dealers don’t even bother to fight over turf…There are plenty of customers to go around,” law officials of a particular town told the publication STAT.
On the streets: A 32-year-old former aircraft technician and his girlfriend, both addicted to heroin, live and sleep under a bridge in Philadelphia, Pennsylvania (July 12, 2016). The city has a growing population of heroin addicts.
The town’s director of the drug task force added, “There’s too much money to be made.”
The same article noted that the town’s 17 officers are overwhelmed dealing with overdoses and petty drug crimes. They simply do not have the resources to fight back.
In an effort to stay a step ahead of authorities, dealers not only sell heroin on street corners but also through advanced distribution networks. Ordering a “hit” is now as easy as ordering a pizza or buying clothing on a smartphone!
“It’s a highly evolved network that allows users to buy heroin without leaving the comfort of their homes,” Newsday reported the executive director of a New York-based nonprofit committed to fighting substance abuse as saying. “You’re dealing with a generation that’s conditioned to instant gratification, and the dealers are taking advantage of that.”
Ripple Effects
Technology has also played a role in putting a new face on the heroin crisis.
Last autumn, a picture of a couple who overdosed in the front seat of their SUV made its way around social media. The most sickening part about the photo was the blank stare of a four-year-old boy sitting in the back seat, who presumably witnessed all that transpired. Authorities who released the photo did so on the grounds that “it is time that the non-drug using public sees what we are now dealing with on a daily basis” (STAT).
For many, the little face peering from the backseat of the car made heroin abuse more real. Yet the photo was just a glimpse into what occurred at the scene. Reports revealed that the distressing image was merely the finale of a death-defying spectacle. Law enforcement officials recounted: “A school bus was making its way down St. Clair Avenue, stopping now and then to let off children. The Ford Explorer was just behind it, weaving erratically. Now, abruptly, the driver hit the brakes. The SUV skidded across the pavement—narrowly missing the bus. It drifted at an angle onto Prospect Street and came to rest near the spot where the children had disembarked, steps from a church” (ibid.).
A police officer who witnessed the entire event reported that when he approached the vehicle the driver’s “head was bobbing back and forth. His pupils were pinpricks. His speech was almost unintelligible.”
The officer says the man then reached for the gearshift and mumbled something about taking his unconscious female passenger to the hospital. This prompted the officer to lean in and snatch the keys from the ignition. While doing so, he noticed the boy in the back seat.
“At that moment,” the story continued, the driver “went completely unconscious” while the woman, “the boy’s grandmother and legal guardian, was ‘turning blue.’”
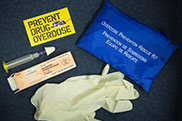
Lifesaving drug: Kits of naloxone are used by emergency personnel when dealing with cases of heroin overdose. A state law, which went into effect in October 2016, requires all Connecticut towns to equip their first responder agencies with the drug.
After backup and medical support arrived, the picture was taken to use as evidence in court. The photographer, a 24-year police force veteran, admitted that as he looked through the lens, he could not help but to think of the child.
“He never said a word,” the photographer told the news outlet. “To this day I have not heard his voice.”
“Just seeing that blank, emotionless expression on his face—it spoke for itself,” he continued.
According to officials, heroin laced with fentanyl was to blame for the whole ordeal. Often called heroin’s synthetic cousin, fentanyl is just one example of a trend in which users are experimenting with more potent chemicals, leading to more overdoses and, sadly, more deaths.
Examples of this are difficult to hear. A five-month old girl from Pennsylvania starved to death in her crib after her parents, in their 20s, fatally overdosed on fentanyl. The coroner believes the child survived alone in her bed for three or four days after her parent’s death before eventually succumbing to a lack of food and water. All three bodies were discovered by a neighbor.
Police and paramedics report that it is not unusual to get called to a residence where multiple family members have overdosed. They say that such calls due to heroin and other powerful opioids are mounting. In one community where overdose calls are twice the number of all other medical calls combined, carfentanil—an elephant tranquilizer—is to blame.
The heroin-carfentanil concoction is so intense—10,000 times more powerful than morphine!—that it can take multiple doses of the heroin antidote Narcan (or naloxone) to revive an overdose victim.
The cost to communities for this life-saving remedy is growing as the desire for an increased high spins out of control.
“A dose of Narcan would usually revive [a] person and bring them back. What we are noticing now is our paramedics sometimes use between four and six, maybe seven doses of the Narcan to revive them, so it is a lot stronger and it has taken a lot more,” a police official told Fox 8 Cleveland.
Even after being revived, victims cannot seem to be scared out of overdosing again. One health official told STAT that he had witnessed people overdose, be revived, then show up again the next day, blue in the face from another overdose.
One of the saddest parts, though, is the fact that many of them are parents, which, he said, seems irrelevant to those who are hopelessly hooked.
“When they are looking at their children, and their children are not enough to make them stop, what really can you say to them?” he told STAT.
These are just some of the awful details of what leaders and other official face. Addicts, no matter how hard they try, cannot get clean. Even those who have gone months or years without abusing often fall back into the trap of dependence. Those charged with resolving the crisis are left to throw all sorts of ideas at the wall in hopes of pinpointing a solution that finally sticks.
Harm Reduction
An emerging trend in combatting heroin addiction is to replace the traditional approach of abstinence—which involves a complete cessation of heroin use by addicts—with that of “harm reduction.”
Two versions of this controversial approach are often used to combat abuse. One involves lessening the usage of the harmful substance with the goal of slowly reducing dependence. The second involves decreasing the “surrounding effects” of drug addiction—without reducing the use of the harmful substance itself.
Methadone clinics are a good example of the first version of harm reduction therapy. Methadone is a synthetic opiate shown to reduce heroin withdrawal symptoms for 24 to 36 hours per dose. The medication, usually dispensed in liquid form, is taken once per day and only available through licensed clinics. Those in treatment, which can go on for years, say that methadone drastically reduces their chance of relapse and is often the bridge they need to slowly wean themselves off heroin.
But these clinics, which are beginning to treat those hooked to opioid-based pain meds as well, are not a panacea. Depending on the clinic’s location, addicts may have to travel great distances to receive their daily dosage. And as the number of patients treated by clinics grows, addicts find it more difficult to make treatment a part of their daily routines.
“Like the morning rush at a Starbucks cafe, cars, pickups and sport utility vehicles start packing into the Volunteer Treatment Center’s parking lots while it’s still dark,” Times Free Press reported. “The clinic…opens at 5:30 a.m. seven days a week. Drug treatment clinics open early in the morning so that patients can take their medicine before work. Patients line up inside the clinic and watch red and green lights over a row of private booths staffed by licensed practical nurses.
“When one patient is done, the green light comes on and the next person enters and closes the door…[Through] an opening in a window inside the booth, the nurse hands over the methadone…in tablet or liquid form. The nurse makes sure the patient downs the dose. Traveling to the clinic every morning to take methadone isn’t convenient for most patients.”
Perhaps the biggest challenge with methadone clinics, however, is that most people simply do not want them in their neighborhoods. There is a negative stigma attached to having a drug clinic in the community and most facilities are prone to loitering addicts who commit other crimes such as theft.
Another harm reduction approach is known as Law Enforcement Assisted Diversion (LEAD). According to the program’s website, it “allows law enforcement officers to redirect low-level offenders engaged in drug or prostitution activity to community-based services, instead of jail and prosecution.”
Under the LEAD program, city government officials, police officers, prosecutors and social workers work closely together to keep addicts out of the criminal justice system. Participants receive food, clothing, shelter and job training. Those administering the program say relapses are expected.
Naturally, many are concerned that programs like LEAD enable addicts and do not incentivize change. They assert the program stops just short of the decriminalization of heroin. Proponents of the program say they want to keep addicts safe until they are ready to change.
Another concern with LEAD is cost. The program started up with $4 million in private funding in the city of Seattle alone, which covered about 300 participants. Yet private money ran out in 2015, leaving taxpayers to fill the gap. Opponents believe that implementing a similar program with many times this number of addicts across the country may not be sustainable.
At the far end of the harm reduction approach is the call for supervised heroin injection sites. This means users would take heroin at taxpayer-funded facilities where a nurse would supervise—and be available to deliver an overdose antidote if necessary. Those promoting the program say the facilities would offer clean needles and access to treatment and recovery programs.
These heroin injection sites, already implemented in Canada, Australia and parts of Europe, have received mixed reviews. A major problem is that facility officials turn a blind eye to illegal drug use. There is also the risk of facilities being exposed to lawsuits in the case of death or serious injury.
Some government officials say it is worth the risk given all the ancillary problems associated with heroin addiction. They believe they can avoid many of the necessary legal and political hurdles for approval if heroin addiction were to be designated an “epidemic” by state health officials.
Opponents remain adamant, however, that these supervised facilities are a bad idea.
“The goal here should be getting people off drugs, not doing what we can to make it easy for people to continue to do them,” an attorney and adviser for Drug Free America Foundation, Inc. told Fox News.
Another panelist added: “In a way it is giving up on these heroin addicts, in the short term maybe they are giving up the dirty needles, but are they really addressing the underlying cause of the addiction, figuring out a way to get sober?”
Mankind’s Conundrum
People are inclined to abuse drugs for varying reasons. Often a person begins to use them to simply alleviate pain from injury or illness. Others seek them as an escape from troubles. Initial drug use also often involves peer pressure, experimentation, seeking recreation, or self-medication.
Regardless, the real problem is addiction and all the negative effects that flow from it.
Ideally, the best way to avoid heroin addiction is to convince everyone to never start. Yet this is an impossible scenario.
While mankind has the ability to make incredible advancements in science, and technology, it does not have the ability to solve the kinds of problems, such as the modern drug dilemma, which it faces.
Consider this quote from Why Man Cannot Solve His Problems written by David C. Pack, publisher/editor-in-chief of this magazine: “Men have created many amazing technological inventions, but they cannot create solutions to their problems. Mankind has harnessed the power of computers to help process vast amounts of information, but human beings cannot correctly process their personal problems. Scientists have discovered much about the size, magnificence and precision of the universe, but they cannot discover the way to peace. Astronomers can find majestic, beautiful new galaxies throughout the universe, but they cannot find a way to preserve the beauty and majesty of earth. Scientists have also unleashed the power of the atom, but they are powerless to unleash answers to life’s greatest questions. Educators have taught millions how to earn a living, but not how to live.”
Mr. Pack continued by repeating and elaborating on a little-known but important principle from the biblical prophet Jeremiah: “O Lord, I know that the way of man is not in himself: it is not in man that walks to direct his steps” (10:23).
“This is another incredible statement,” Mr. Pack continues. “When confronted with problems or important decisions, men simply do not know what to do! They are at a loss for how to correctly address and solve the challenges, difficulties and problems they face in their personal lives.”
As powerful and knowledgeable as man is, he is ultimately unable to direct his own steps. Yes, his knowledge has gotten him far, but there are certain problems that even he cannot overcome.
The heroin crisis is a prime example. Heroin and other drug abuse has become so out of control that we have resorted to just letting it go. Though programs like “harm reduction” have the sincere goal of helping people, they are just fancy-sounding ways of allowing drug abuse to continue since it cannot be stopped.
Solutions for the heroin problem are beyond our capacity. While this article does not discuss resolving the crisis, Mr. Pack’s book reveals how it will eventually be stopped and how those now experiencing addiction will one day find the happiness and satisfaction that they so strongly desire.
To learn more, read Why Man Cannot Solve His Problems. The ultimate solution is just over the horizon.
 Andrew Burton/Getty Images
Andrew Burton/Getty Images