 CDC via AP
CDC via AP
World News Desk
Learn the why behind the headlines.
Subscribe to the Real Truth for FREE news and analysis.
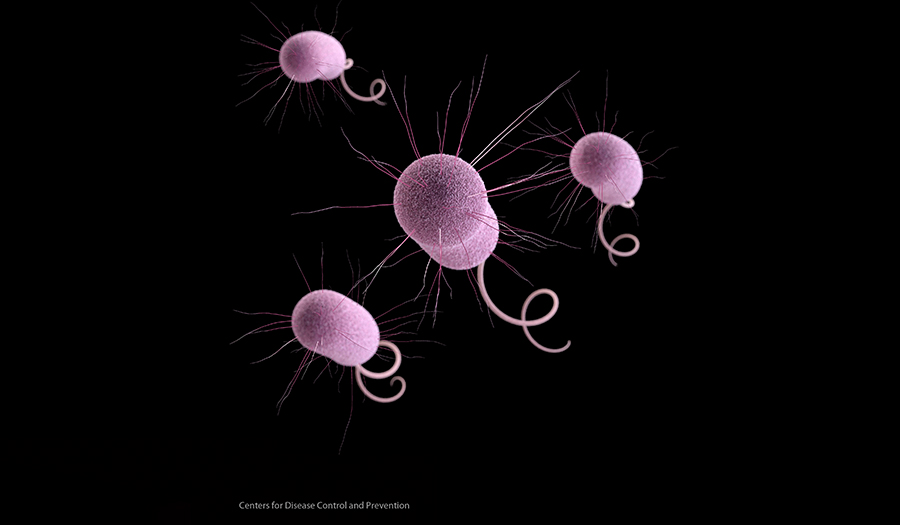
Subscribe NowBacteria with an unusual resistance to last-resort antibiotics were found 221 times in the United States during nationwide testing in 2017, the Centers of Disease Control and Prevention reported.
“Nightmare bacteria,” as it has been labeled by CDC, mostly strikes people in hospitals and nursing homes who need IVs and other tubes that can get infected. Though it has not spread widely, the risk of an outbreak is high as 1 in 10 cases of those infected with the superbugs showed no symptoms.
Some of the sick patients had traveled for surgery or other healthcare to another country where drug-resistant germs are more common, and the superbug infections were discovered after they returned to the U.S.
“These verge on untreatable infections” where the only option may be supportive care—fluids and sometimes machines to maintain life to give the patient a chance to recover, said Dr. Anne Schuchat, principal deputy director of the CDC.
Last year, public health labs around the country were asked to watch for and quickly respond to cases of advanced antibiotic resistance, especially to some last-resort antibiotics called carbapenems.
In the first nine months of the year, more than 5,770 samples were tested for these “nightmare bacteria,” and one quarter were found to have genes that make them hard to treat and easy to share their resistance tricks with other types of bacteria. Of these, 221 had unusual genes that conferred resistance. The cases were scattered throughout 27 states.
“Even in remote areas” this threat is real, because patients often transfer to and from other places for care, said Dr. Jay Butler, chief medical officer for the state of Alaska.
Others in close contact with the infected patient then were tested, and 11 percent were found to be carrying the same superbugs even though they were not sick.
“It’s already happened several times in the U.S.—and when one superbug gives new powers to a different superbug, the result can be an infection that is impossible to treat,” CBS News reported.
“Once antibiotic resistance spreads, it is harder to control—like a wildfire,” the CDC said in a statement.
The superbug “wasn’t just a problem in one or two states,” Dr. Schuchat said according to CNN. She added that “the 221 rare genes were found in isolates gathered in 27 states from infection samples that included pneumonia, bloodstream infections and urinary tract infections,” the news agency reported.
Bugs and drugs are in a constant battle, as germs evolve to resist new and old antibiotics. About 2 million Americans get infections from antibiotic-resistant bacteria each year and 23,000 die.
The overuse of antibacterial medicines for viral infections is a major factor.
Dr. Lance Price, director of the Antibiotic Resistance Action Center at George Washington University, told NBC News that doctors “who want good ratings give patients what they demand: a prescription, even though antibiotics do not help viral infections and are helping drive the evolution of superbugs.”
This article contains information from The Associated Press.
More on Related Topics:
- Afghan Hunger Crisis Deepens as Aid Funding Falls Short, UN Says
- Israel’s Longest War Is Leaving a Trail of Traumatized Soldiers, With Suicides Also on the Rise
- Maintaining Your Health as You Grow Older
- The Blind to See—Humanity’s Fight to Cure Blindness
- ‘Nightmare Bacteria’ Cases Are Increasing in the U.S.


