 National Institute of Allergy and Infectious Diseases
National Institute of Allergy and Infectious Diseases
World News Desk
Learn the why behind the headlines.
Subscribe to the Real Truth for FREE news and analysis.
Subscribe NowBacteria can genetically develop resistance to antibiotics it has not encountered before, a study by doctors Catriona Harkins and Matthew Holden at the University of St. Andrews in the United Kingdom showed.
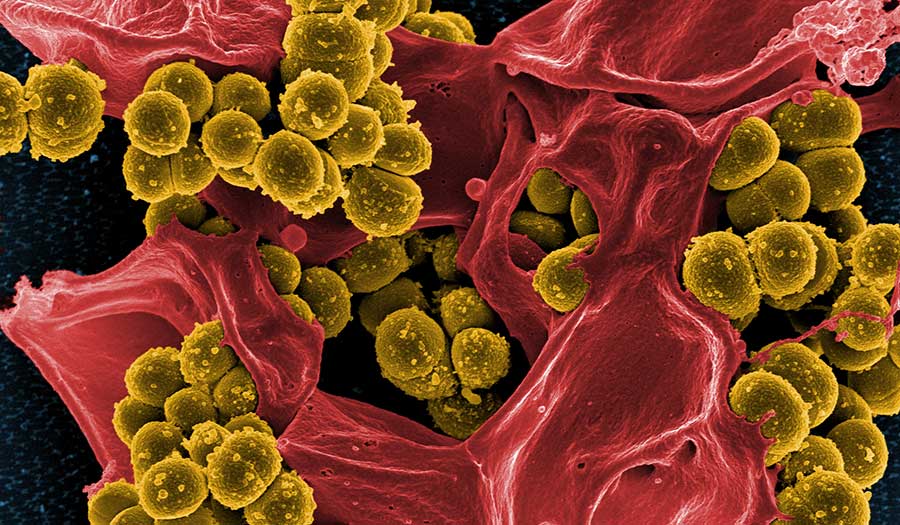
The finding explains why the first cases of methicillin-resistant Staphylococcus aureus (MRSA) all occurred in patients that had not been exposed to methicillin. It also explains why strains of MRSA appeared in Eastern Europe and India where methicillin had not been used previously.
As part of their research, the team of doctors studied the DNA of MRSA bacteria samples collected between 1960 and 1989.
“By comparing these strains and reconstructing their evolutionary history, the team calculated that they all descended from a common ancestor that first acquired the ability to resist methicillin in 1946—13 years before people started using the drug to treat infections,” The Atlantic reported.
“So bacteria can begin evolving resistance to antibiotics that they haven’t even encountered yet,” the publication summarized based on the study’s findings. “And new drugs can be neutralized by adaptive genes that are lurking in the environment, waiting for the chance to rise to the occasion.”
The study’s researchers were not the first to discover that bacteria are capable of “learning” resistance to antibiotics before being exposed to them. According to another finding published in The Lancet Infectious Diseases journal, 11 different types of bacteria are capable of sharing genes that “teach” them to resist antibiotics they have never encountered.
The Texas Medical Center in Houston—the world’s largest medical center—announced in May 2017 the detection of klebsiella CG307, a deadly bacterium able to absorb genes from other bacteria so that it can resist antibiotics it has never encountered.
“In other words, bacteria are actively trading a toolkit that makes them both deadly and resistant to treatment,” NBC News explained. “The discovery in Houston, a diverse city of 6 million people that’s also a popular destination for people seeking medical treatment, is especially troubling, the researchers noted.”
Dr. James Musser, who works at the medical center, said in an interview for a PBS Frontline episode that “as more resistance occurs—and I mean nationally, not just in our hospital—there’s more of a probability of creating an organism that is now resistant to every antibiotic.”
In a society where so many people rely on antibiotics, not having them available seems inconceivable, the PBS interviewer stated.
“The prospect of life without antibiotics is barely imaginable for a world that has had a cheap and plentiful supply of them since the end of World War II. They are a staple of modern medicine. It’s hard to recall a time without them, when an infected cut could kill a healthy young person in a matter of days.
“But it’s now clear that we are heading back in that direction, that the miracle of these drugs is slipping away.”
More on Related Topics:
- Afghan Hunger Crisis Deepens as Aid Funding Falls Short, UN Says
- Israel’s Longest War Is Leaving a Trail of Traumatized Soldiers, With Suicides Also on the Rise
- Maintaining Your Health as You Grow Older
- The Blind to See—Humanity’s Fight to Cure Blindness
- ‘Nightmare Bacteria’ Cases Are Increasing in the U.S.


