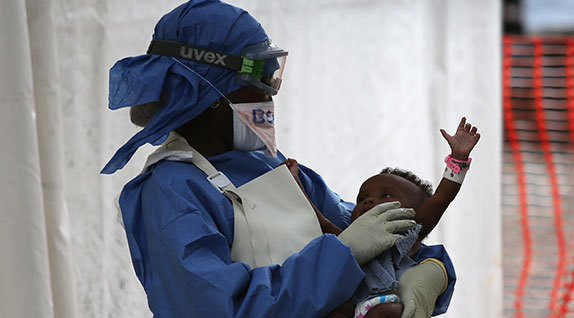
 John Moore/Getty Images
John Moore/Getty Images
Article
Approximately one year after Ebola took the lives of over 11,000 people and infected approximately 29,000, health experts, scientists and concerned citizens are contemplating how prepared we are for the next large-scale outbreak.
Learn the why behind the headlines.
Subscribe to the Real Truth for FREE news and analysis.
Subscribe NowThe haunting images of mass graves filled with nameless body bags, children hooked to IVs, family members wailing over deceased loved ones, and heartrending stories of orphaned children that flooded newspapers starting in March 2014 made it clear that humanity was facing a different kind of epidemic—with a mortality rate that at its highest killed 70 percent of its victims.
The Ebola strain, which was first contracted by an 18-month-old boy in Meliandou, Guinea, from supposed contact with bats, quickly spread throughout his family, killing all but his father.
The virus picked up speed as it traveled through neighboring Liberia and Sierra Leone. Within just three months of it taking hold, it had killed 300 people and infected more than 500.
As summer turned to fall, countries including Nigeria, Senegal, Spain and Mali harbored cases and travelers from the United Kingdom to Hong Kong presented symptoms. A separate strain even began affecting those in the Democratic Republic of Congo.
For the first time, Ebola also reached the shores of the United States when a man, who traveled from Liberia with no symptoms, fell ill within days of entering the country. Doctors confirmed the patient’s symptoms as Ebola, and isolated him. He died several days later.
Two healthcare workers who cared for him also contracted the disease, sparking panic among U.S. citizens. Local news stations featured how-to-handle-Ebola segments and even went so far as to interview veterinarians on whether pets could contract it.
Despite hand-wringing over the possible spread, less than 20 people were transported to the U.S. for treatment of Ebola or became infected with it. Out of those, only two died.
The outbreak, though, set the world on edge. Newspapers questioned if this could be the “big one” that many had anticipated. Country after country reported infections, and nations contemplated prohibiting travel to affected areas. It seemed only a matter of time before great numbers across the entire world contracted it.
Yet within a year, the epidemic seemingly stopped as suddenly as it came and most turned their attention back to their daily activities. The virus that had once splashed its name across every newspaper and magazine became more of a distant memory to all but those left to pick up the pieces.
Front Lines
Liberian native and trained neurosurgeon Dr. Jerry Brown understands the reality of Ebola’s effects all too well. The year the epidemic hit, Dr. Brown accepted a position as Medical Director of the Eternal Love Winning Africa Hospital (ELWA) in the nation’s capital of Monrovia.
On March 28, 2014, his hospital staff met for the first time to discuss the virus. At the time, it was only in Guinea—but Dr. Brown saw its potential to spread. He immediately began training personnel on infection prevention since it was the first time that Ebola had surfaced in West Africa.
 The Real Truth
The Real Truth“People never knew what disease they were dealing with,” he said during a speech and panel discussion on Ebola preparedness at Case Western Reserve University in Cleveland, Ohio. “They had no knowledge of it.”
During the event, which was attended by Real Truth staff, Dr. Brown explained that he turned ELWA’s small on-site chapel into the nation’s first Ebola Treatment Unit (ETU). It could hold five people.
His preparation paid off. By the time the first case occurred in Liberia on March 30, he felt he was somewhat ready.
But he soon found himself struggling to find enough room to fit all the patients that came to the hospital starting on April 12.
As more arrived for treatment, Dr. Brown had to branch into a kitchen and laundry facility, where he set up 20 more beds for an ETU. Patients reached the hospital by any means possible—ambulance, taxi, motorcycle, or were brought in by a loved one, he recounted. Eventually, with increasing numbers contracting Ebola, he was able to acquire enough extension tents to set around the hospital with the capacity to hold 100.
Retaining and recruiting staff was difficult. Many were terrified of the disease and did not want to become casualties. Even contact tracers, who were hired to identify those who had come into contact with Ebola victims, were scared for their lives.
“They themselves were afraid of going into the communities for fear of the disease,” he said.
His clinic found itself reaching out to the public for monetary support. He went on the radio to ask citizens to help gather needed supplies.
While this yielded results, life on the ground turned chaotic. International aid came, but in some cases it was too little, too late. Ebola was running rampant, with seemingly no hope of stopping.
Bodies began to pile up. On August 6, Liberian President Ellen Johnson Sirleaf declared a three-month state of emergency, which included market closings, curfews and restricting the movement of patients and anyone who had contact with them. The government also mandated that anyone who died from Ebola be cremated. Tens of thousands of people were quarantined and even coastal areas were blocked off. The moves resulted in riots and widespread looting.
The disunity of international efforts did not help the process. Dr. Brown explained that various organizations and health teams from different countries rarely worked together, and instead each wanted to take sole credit for their efforts.
Because there was not a coordinated plan on how international aid would be distributed in the nation, some hospitals, including Dr. Brown’s, did not have adequate supplies to combat the disease.
For example, he explained that the ETU next door “had a stockpile of IV fluids and anything they wanted. But when you came to our ETU, we had to look for foot covers. We couldn’t find foot covers so we waited…and bought plastic bags and covered our feet in order to work.”
The stigma of the disease and lack of knowledge about it caused further deaths. Those who had never heard of it thought Western health officials who donned protective suits were extracting the organs of those who went to the ETU, Dr. Brown said. Therefore, family members hid decaying corpses in their homes or buried them before health officials could find them, which only worsened the epidemic.
“…instead of showing up for treatment, they chose to remain home,” he said. “And that led to a rapid spread and increased mortality.”
Dr. Brown said another struggle was that there was “an acute shortage of trained manpower to handle the crisis we had initially. In addition to that, a lot of our trained manpower who trained physicians who started the fight died. You know, the infectious disease doctor in Sierra Leone, he died. We lost two internists, the only two laboratory attendants we had in Liberia died as a result of the disease.”
Even though Liberia had the highest number of healthcare workers infected by the end of the epidemic, due to his efforts to identify and contain Ebola, not one member of Dr. Brown’s staff died from it.
Different From Before
While various strains of Ebola have surfaced in small towns across Central Africa since its initial discovery in 1976, the year 2014 was the first time it hit a heavily populated area.
“This was more urban-based in many ways than the other outbreaks that were in remote and rural areas,” Dr. Robert Salata, a professor of medicine, epidemiology and international health at Case Western Reserve University, said during the panel discussion. He explained that in previous outbreaks, the disease was contained to smaller rural areas because those who contracted it died before they had a chance to spread it to surrounding regions.
 Cellou Binani/AFP/Getty Images
Cellou Binani/AFP/Getty ImagesJohn Dye, Viral Immunology Branch Chief of the U.S. Army Medical Research Institute of Infectious Diseases, concurred that the epidemic was definitely unique.
“Ebola has been popping up all over Central Africa for decades and the difference with this outbreak is that, for instance, if you compare it to Uganda, we’re talking about dozens of cases as opposed to tens of thousands,” he said. “The difference is that Uganda had seen it before. And it had never been seen in West Africa, except one case in Cote d’Ivoire and it was believed to have actually migrated to Cote d’Ivoire from Central Africa…”
At first, he said, Ebola was hard to diagnose as “with the general symptoms…general malaise, you can’t really put your finger on it. It was probably early diagnosed as Lassa virus would be my guess because the symptoms are so similar.”
It was also the first time that those from outside Africa were infected, Mr. Dye said, which could provide clues in the future as to how the disease affects those not currently infected with any other kind of malady. At least 75 percent of survivors complain of backaches, arthritis, headaches, sleep apnea, and vision issues. Yet 95 percent of them become infected with malaria due to a weakened immune system after they contract Ebola, known as sequela, or a condition that surfaces as a consequence of a previous disease or infection, he said.
“It’s very difficult because in Africa, you’re constantly barraged by all kinds of pathogens,” he said, later stating, “What’s different about this outbreak is that Westerners have been infected and they have come back to industrialized nations where they are receiving top healthcare and yet you are now seeing sequela.”
According to Mr. Dye, Ebola survivors have “gold in their blood,” and studying them is key to combatting the virus.
Economic Impact
An often overlooked aspect of disease epidemics is the fiscal impact on developing countries such as Sierra Leone, Guinea and Liberia—which all have some of the highest poverty rates in the world.
“Their public health infrastructure was poor to begin with,” Craig Giesze, a senior operations officer for the World Bank Group in Dakar, Senegal, told the panel regarding Liberia. “Imagine what it is like now.”
Mr. Giesze said that the latest epidemic may have set some of the countries, including Liberia, “back 10 years in their economic development.”
“Even though they’ve made improvements and they have contained Ebola much more effectively than at the beginning, foreign investors…aren’t buying it,” he said. “And basically markets work because there is confidence. And as of right now, there is a gap in confidence…”
According to World Vision, due to a continuing civil war, around 70 percent of Sierra Leone’s six million citizens live below the poverty line. It has one of the highest rates of mortality in children under 5 and only half the population in urban areas has a safe water supply. Electricity is almost non-existent.
Likewise, Liberia is classified as a “low income country that relies heavily on foreign assistance,” according to The World Factbook. It was ranked as the fourth poorest country in the world by Global Finance magazine. Since 2003, it has also been rebuilding from a 14-year civil war.
Guinea struggles with its own problems. It was ranked as Earth’s ninth poorest country with half the population living below the poverty line.
“Food insecurity and malnutrition among children are widespread,” the International Fund for Agricultural Development reported.
Mr. Giesze said it will be difficult to prepare countries in such circumstances for future outbreaks, but he and other organizations are trying to dialogue more efficiently with coalitions such as the Economic Community of West African States and the African Development Bank.
“I think that if we just take a step back, though, we still have a long way to go because we know that just across the board, health infrastructure is still substandard in West Africa,” he said.
Zoonotic Base
While Ebola was contained, experts caution that we are not out of the woods yet. History as a guide shows that there is always something that surfaces. Disease in its many forms continues to run rampant, spurred on by new pathogens carried to humans. And it is often when it is least expected that a new strain or virus will appear out of a faraway forest or some other remote area.
“Nearly 75 percent of all new, emerging, or re-emerging diseases affecting humans at the beginning of the 21st century are zoonotic (i.e. originated in animals),” USAID reported in a document titled “Emerging Pandemic Threats.” “Notable reminders of how vulnerable the increasingly interconnected world is to the global impact of new emergent diseases include HIV/AIDS, severe acute respiratory syndrome (SARS), the H5N1 strain of avian influenza, and the 2009 pandemic H1N1 influenza virus. The speed with which these diseases can emerge and spread presents serious public health, economic, and development concerns. It also underscores the need for the development of comprehensive disease detection and response capacities, particularly in ‘hot spot’ areas such as central Africa, South and Southeast Asia, and Latin America where a confluence of risk factors may contribute to disease emergence.”
Many of the worst diseases in history have been zoonotic. The Centers for Disease Control and Prevention estimates that over six of every 10 infectious diseases are spread from animals. Since 1940, it is estimated that over 300 new diseases have been identified.
In addition, “Three of the top ten causes of death, or sixteen percent of all deaths each year, are from infectious diseases,” according to the Center for Strategic and International Studies. “Most of these deaths are in low- and middle-income countries and are attributable to preventable or treatable diseases such as diarrhea, lower respiratory infections, HIV/AIDS, tuberculosis, and malaria. While significant advances have been made in interventions to prevent and treat most of these diseases, those interventions are often unavailable to the populations most in need.”
“Infectious diseases have been an ever-present threat to mankind,” the organization reported. “From the biblical plagues and the Plague of Athens in ancient times, to the Black Death of the Middle Ages, the 1918 ‘Spanish Flu’ pandemic, and more recently, the HIV/AIDS pandemic, infectious diseases have continued to emerge and reemerge in a manner that defies accurate predictions.”
Worst in History
One of the first and most deadly pandemics recorded was the Plague of Justinian, a bubonic plague that spread across the Eastern Roman Empire from AD 541 to 542. The disease, which was likely carried by rats on boats transporting grain from Egypt to Constantinople, was so devastating that it halted the empire’s military operations. The CDC estimates that it killed over 100 million people in and around the Mediterranean region.
Less than a millennium later, the bubonic plague outbreak—notoriously labeled the Black Plague—was brought from Asia to Europe via fleas living on black rats in merchant ships. The plague continued to reach further north in Europe and Russia until it phased out in 1353. By then, it had taken the lives of 75 million people, roughly wiping out one quarter of the world population at the time.
Massive pandemics continued to hit the world after the Industrial Revolution and advancement in medical understanding. The 19th century hosted three cholera outbreaks, with the second—occurring from 1829 to 1851—being the most deadly of any disease in the same century.
Since then, there have been eight cholera outbreaks. The World Health Organization reports the disease still kills as many as 120,000 each year.
Another deadly pandemic occurred at the end of the first world war—Spanish influenza. Brought to the U.S. by troops returning from Europe in March 1918, within two years, the flu left over half a million Americans dead, countless orphans, vacant jobs, and closed businesses. The pandemic affected every nation on Earth, killing 50 to 100 million and infecting 500 million worldwide.
Various influenzas have also taken root in the last 50 or so years. The Asian flu of 1957 was believed to have been spread by wild ducks. While it was the least severe of the three influenza pandemics of the 20th century, it still killed two million. Unlike Spanish influenza, the quick development of a vaccine prevented the Asian flu from causing a much more massive death toll.
The Hong Kong flu of 1968-1969 caused between one and four million deaths worldwide. It reached the United States through soldiers returning to California from Vietnam.
More recently, the swine flu pandemic of 2009 scared the 21st-century world. It broke out in March of that year when H1N1, the same virus that caused the Spanish influenza in 1918, infected 60 percent of the town of La Gloria, Mexico.
From there, it spread throughout Mexico and the United States until the WHO’s director-general declared it a “public health emergency of international concern.” Only days after the warning, swine flu cases were confirmed in Canada, the United Kingdom, Israel, New Zealand, Continental Europe, East Asia, South America, and Africa.
After the pandemic was declared over on August 10, 2010, it was estimated that anywhere from 10 to 200 million had been infected. The WHO confirmed that 18,500 had died from the disease.
Several other diseases have not had pandemic outbreaks as has occurred with malaria, a mosquito-borne illness that kills one to three million per year, but have the potential to be just as deadly. During the 20th century alone, the illness killed between 300 and 500 million people.
“Humanity is locked in a millennia-old battle to the death with diseases like these,” The Guardian reported. “We have fought them back with herculean effort. We developed penicillin and other antibiotics to treat bacteria like the ones thought responsible for the Black Death, and vaccines to fight viruses.
“But we are in an arms race. And while our ability to treat disease is better than ever before, the current outbreak of Ebola, and the first diagnosis of the virus outside of Africa, is reminding us that as our cities get bigger and international travel becomes easier, the risks involved in an outbreak grow ever higher.”
Pandemic Spread
While an epidemic hit Africa this time, next time, it could be somewhere else—and in another form.
Imagine, for example, that a contagious airborne disease suddenly surfaced, a nightmare scenario according to health experts.
“Even with modern medicine, we haven’t rid ourselves of pandemics; indeed, they have sprung up far more recently than 1918,” The Guardian reported. “HIV/Aids is the most recent truly devastating pandemic—and H5N1 avian flu was even more widespread, though less deadly.
“There are many nightmare scenarios, according to Robert G Webster, chair of the virology division at St Jude children’s research hospital. ‘Just imagine if the Ebola outbreak in West Africa was transmitted by aerosol. If flu was just as lethal. If H5N1 [avian flu] was as lethal in humans as it is in chickens—and studies have shown that it only takes about three mutations to make it highly lethal. It’s not out of the realms of possibility.’”
Ebola will most likely never become airborne, according to the CDC, as it can only be transmitted by direct contact with bodily fluids. However, another type of hemorrhagic fever or a particularly virulent strain of influenza could.
Influenza is at the top of the list of concern due to its airborne capacity, even in countries with the capability to fight it. In the United States, vaccines must be created a year in advance, so it is necessary for health officials to guess the viruses that could become problems and create vaccines based on those, which is often not effective. During the 2014-2015 flu season, for example, the vaccine was only 20 percent effective against circulating flu strains.
“Experts must pick which viruses to include in the vaccine many months in advance in order for vaccine to be produced and delivered on time,” the CDC stated on their website. “And flu viruses change constantly (called drift); they can change from one season to the next or they can even change within the course of one flu season. Because of these factors, there is always the possibility of a less than optimal match between circulating viruses and the viruses in the vaccine.”
If there was a sudden flu pandemic, however, the CDC said in a handout that seasonal flu shots would be worthless.
“Because the pandemic flu virus will be new to people, many people could get very sick or could die. Seasonal flu shots do not protect people from pandemic flu.”
The organization acknowledged that such a pandemic could be imminent: “Public health experts say it’s not a matter of IF a flu pandemic will happen, but WHEN. We cannot predict when the next flu pandemic will happen.”
In other countries, such as India, which is home to over 1.25 billion people, a disease such as cholera, malaria or dengue fever, is of greater concern. The nation has repeatedly suffered the greatest proportion of deaths in each worldwide pandemic. For instance, the Spanish influenza killed 17 million Indians, representing at least 17 percent of the worldwide total and five percent of the country’s population at the time.
Concerns that this could happen again have reemerged. Earlier in the year, an outbreak of a strand of malaria resistant to artemisinin, the antibiotic that has prevented the illness from killing millions of people since its development, emerged in Southeast Asia and crept within 15 miles of India’s border. It is believed that if the disease, which takes the lives of over 580,000 people a year worldwide, entered the nation, little could be done to control the spread.
Nearly six million new cases of dengue fever occur each year in India—the largest number of cases in the world.
“This is due, in part, to India’s large population,” Doctor Donald Shepard explained in a Deutsche Welle article. “In incidence rates per population, parts of Southeast Asia and South America are highest.”
“However, due to growing urban populations and travel in India, the country’s incidence rates are substantial. Without additional control measures, numbers of cases are likely to continue to increase.”
The greatest concern is the fact that India consumes the most antibiotics of any country, causing the highest number of cases of drug-resistant diseases.
Economist Jim O’Neill, who is chairman of the Review on Antimicrobial Resistance, said that by 2050, India could see two million more deaths per year due to superbugs. Also, drug-resistant infections could spread from there, causing an estimated 10 million more deaths worldwide per year and a greater chance of pandemics.
“Current antibiotics are becoming increasingly ineffective, not only at fighting common illnesses like pneumonia and urinary tract infections, but also at treating a range of infections, such as tuberculosis and malaria, which now risk again becoming incurable,” he wrote in an article for Project Syndicate.
Repeated in History
So far, it appears that man has been holding back the floodgates of disease. But it is not all his doing. Many of the severest outbreaks of the past simply ran their course. Preventative measures do help end epidemics, but they often simply die out on their own.
Even with modern medicine, man does not yet possess the resources to deal with such large-scale epidemics. This was witnessed during the 2009 swine flu pandemic and later Ebola outbreak.
Following the swine flu outbreak, Dr. Harvey Fineberg wrote in an assessment of the pandemic’s handling: “Pandemics can be fearsome teachers. No matter what one believes about the response to the 2009 pandemic by WHO and other authorities, all must be grateful that relatively few people died. Influenza viruses are notoriously unpredictable. We were lucky this time but, as the report concludes, the world is ill-prepared for a severe pandemic or for any similarly global, sustained and threatening public-health emergency.”
In addition, the report stated that “the influenza pandemic exposed vulnerabilities in global, national and local public-health capacities, limitations of scientific knowledge, difficulties in decision-making under conditions of uncertainty, complexities in international cooperation and challenges in communication among experts, policy-makers and the public.”
Two years later, a statement by WHO about how it will strive to better itself in the next crisis used the same wording: “The Ebola outbreak that started in December 2013 became a public health, humanitarian and socioeconomic crisis with a devastating impact on families, communities and affected countries. It also served as a reminder that the world, including WHO, is ill-prepared for a large and sustained disease outbreak” (emphasis added).
This illustrates a point: while man can devise vaccines, medicines and methods of social distancing and tracking, he can never totally eradicate illness with these tactics or his own preparation—which means future pandemics are coming—even to Western nations, which may be more difficult to stop. Globalization ensures that coming outbreaks will spread more quickly and not die out easily.
“…this was a devastating epidemic,” Dr. Salata told the audience at the conclusion of the Ebola preparedness panel. “This will occur again…It may be elsewhere. And we’ll see epidemics of other infections and so therefore we have to be more global in our thinking about disease and how that can reach our borders as well.”
More on Related Topics:
- Iran War Is Latest Blow to Somalia’s Malnourished Children
- In a Nigerian Village, Extremists Issued a Call to Prayer and Then Slaughtered Those Who Turned Up
- Sudanese Paramilitary Force Abducting Children in Darfur, Witnesses Say
- Nigeria’s Northeast Faces Worst Hunger in a Decade as Aid Cuts Hit Region, UN Says
- Uganda Shuts Down Internet Ahead of Election, Orders Rights Groups to Halt Work


