 Marine Simon/AFP/Getty Images
Marine Simon/AFP/Getty Images
Article
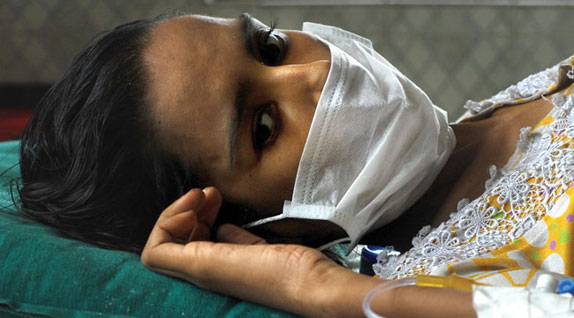
A patient takes antibiotics for a bacterial infection. The bacterium adapts and becomes antibiotic-resistant. Scientists invent stronger drugs. The bacterium morphs to a still stronger strain. After repeating this cycle for over 80 years, is this the end of the antibiotic age? Where else can you turn?
Learn the why behind the headlines.
Subscribe to the Real Truth for FREE news and analysis.
Subscribe NowIn a small, dimly lit hospital chapel, behind the first of four bare wooden pews, a man in his early 30s kneels in front of a cross at the front of the room, head bowed.
After a long moment of silence he thinks, How did we get here? It was supposed to be a routine procedure.
For the first time since he was a child, he prays. Why her? he pleads.
His wife had come in for minor knee surgery. After the seemingly successful procedure, the area around her knee turned black and swollen.
Minutes pass and the man gets up to return to his wife’s side.
Days later, he wheels his wife to the car, a bandage wrapped around the stub of a now amputated leg.
His prayer went unanswered.
This type of story is all too frequent. During surgery, something is left behind—tiny spores of the bacteria called MRSA. This hard-to-cure superbug, which is an extreme staph infection, can infect a patient with sores on the skin, necrotizing pneumonia, and even lead to death. Worse, MRSA can be carried unknowingly on hands, clothes or even a “get well” card tied to a bouquet of flowers.
In past years, this hospital superbug killed more people in America than AIDS. Its cohort, C. difficile, killed about double that amount. For decades, these stubborn bacteria have plagued healthcare facilities. And for decades, physicians have countered with their favorite weapon: antibiotics.
But there is a problem: Each time a person takes antibiotics for these superbugs, the bacteria can mutate and “learn” to resist the powerful antidotes.
During the past 10 years, hospital superbugs have been rampant, with the death toll quietly rising in the very place people go to regain their health—local hospitals.
What are these hospital superbugs? Their scientific names are Clostridium difficile (C. difficile) and methicillin-resistant Staphylococcus aureus (MRSA, pronounced “mersa” for short).
As these bacteria become stronger, doctors use the strongest antibiotics to combat them. But the bacteria continue to adapt, and will soon overtake even the most powerful drugs. What happens when all antibiotic options run out?
Super Impact
According to the Centers for Disease Control and Prevention (CDC), “MRSA occurs most frequently among patients who undergo invasive medical procedures or who have weakened immune systems and are being treated in hospitals and healthcare facilities such as nursing homes and dialysis centers. MRSA in healthcare settings commonly causes serious and potentially life threatening infections, such as bloodstream infections, surgical site infections, or pneumonia.”
As resistance to antibiotics has increased, hospitals have had to turn to “the drug of last resort”—vancomyicin—to combat MRSA.
Regarding C. difficile, the CDC describes it as “a bacterium that causes diarrhea and more serious intestinal conditions such as colitis.” Symptoms include at least three bowel movements per day for two or more days, fever, loss of appetite, nausea, and abdominal pain or tenderness.
An estimated 35,000 C. difficile infections occur per year in American hospitals, and tens of thousands more in nursing homes—with 15,000 to 20,000 killed annually.
The United Kingdom Department of Health recorded 36,674 deaths between 1997 and 2007 for the two infections (C. difficile claimed 26,208 and MRSA 10,466).
Researchers from the University of Nottingham reported, “Official figures show that 5000 people die from a healthcare-associated infection every year in the UK and tackling the super bugs costs the NHS £1bn a year. 1 in 12 of us will pick up an infection during a stay in hospital. There’s a 1 in 77 chance of contracting MRSA and a 1 in 50 chance of developing C. diff.”
An April 2008 CDC report showed that U.S. hospital patient infections doubled from 2001 to 2005. The New York Times reported, “Several years ago, the mortality rate from a C. difficile infection was around 1 to 2 percent. But today, various studies estimate that the death rate is 6 percent. The reason is that a hypervirulent strain has emerged that emits higher levels of toxins than earlier strains.”
More worrisome is that if you have a healthy immune system, you can carry these virulent superbugs and not even know it without a lab test. Doctors can take it into exam rooms, family members can infect a patient they are visiting—even surgeons can carry it into the operating room. Again, these bacteria can sneak in on a nose or hand, and can infect through a wound the size of a mosquito bite.
Growing the Bugs
How did these near unstoppable bacteria grow to such formidable proportions? Through overusing antibiotics.
For each decade following the 1928 invention of penicillin, physicians prescribed antibiotics as a “cure-all” for just about everything: Have an earache? Take some Amoxicillin. Have bronchitis? Try Zithromax. Sinusitis? Trimethoprim-sulfamethoxazole. Won’t go away? Take moxifloxacin; it’s stronger.
Entire generations have been born and bred on this thinking. Nearly every trip to the doctor ends with a stop at the local drugstore—antibiotic prescription in hand.
Now the healthcare industry is reaping the effects of reckless antibiotic overuse. What was once a giant safety net against disease has created monstrous bacteria Clostridium difficile and methicillin-resistant Staphylococcus aureus, among others.
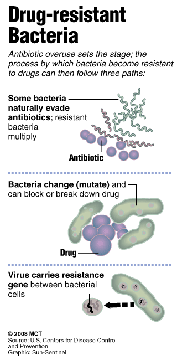
After an unwanted bacterium is introduced to the body, the immune system fights back. Physicians typically prescribe antibiotics (any drug that either kills bacteria or hampers their growth) to aid the immune system.
However, with each use, bacteria can begin to “resist” the drug, using a number of tricks. Some make themselves less permeable and the antibiotic cannot be absorbed. Other bacteria change their structure so that antibiotics no longer recognize and destroy them.
In the worst case, researchers now document bacteria that produce an enzyme to dissolve the antibiotic, rendering it useless. In effect, the hunter antibiotic has become the hunted!
Another danger associated with the misuse of antibiotics is that they destroy bacteria indiscriminately. The body also has healthy bacteria that aid in digestion and help protect the body.
In the case of C. difficile, the bacterium can often survive the initial antibiotics course. This means that once all other bacterial competition is killed off, it can grow and flourish. Often a person will be put on another round of stronger antibiotics—meaning that C. difficile can possibly grow stronger and more resistant as it spreads to new hosts.
Also, scientists are finding that after long courses of antibiotics, C. difficile patients pass the bacterium’s spores into the environment around them—even after treatment has ended and the patient appears symptom-free.
Researchers at the Wellcome Trust Sanger Institute created a “mouse hospital” to simulate the spread of C. difficile in a healthcare environment.
“We treated mice with short and longer courses of antibiotics,” says Professor Gordon Dougan, Head of Pathogen Genetics at the Sanger Institute and senior author on the study. “After a short course most mice had dropped back to normal spore shedding levels around two weeks after cessation of the treatment. But after long term exposure to antibiotics some of the mice remained in their ‘supershedder’ state for weeks or even longer after treatment was stopped. We should consider that patients still pose a considerable transmission threat some weeks after treatment is terminated even if they have not exhibited signs of C. difficile disease.”
Prevention Measures
The towering threat of drug-resistant superbugs has hospital, government and local officials in Britain, the United States and elsewhere scrambling for answers.
One solution is for medical facilities to test everyone for the bugs upon admission, and quarantine those infected. Yet many hospitals are wary of this, fearing potential lawsuits from patients who tested negative when they were admitted, but became infected during their stay.
While implementing more tests and isolating infected patients have shown promising results, the main problem in the superbug fight is the over-prescription of antibiotics. Although researchers have noted a decline in ear infection antibiotic prescriptions, stronger antibiotic types are still regularly overused.
“‘There is good news about declining antibiotic use, since inappropriate use of antibiotics can result in bacteria that are resistant to these antibiotics,’ said Dr. Marie R. Griffin, a professor of preventive medicine at Vanderbilt University Medical Center and a co-author of the study [published in the Journal of the American Medical Association]. ‘However, overuse of powerful antibiotics remains a problem’” (U.S. News and World Report).
But is it too little too late? Even as healthcare facilities work to quell growing outbreaks of MRSA and C. difficile within their walls—the virulent superbugs are increasingly turning up outside their walls in the community. Although researchers have yet to put an accurate number on superbug infections, newspapers regularly report outbreaks in gyms, public pools and high school locker rooms.
Also, as the flu season draws near, scientists fear community-acquired MRSA could team up with the swine flu virus to produce deadly results. Those whose immune systems are weakened by the H1N1 virus are highly susceptible to getting MRSA-induced necrotizing pneumonia.
An infections expert at the University of Nottingham, Professor Richard James told the Telegraph, “The threat from [community-acquired] MRSA in the US is a very serious concern, especially if there is an epidemic. It could trigger a large number of cases of necrotizing pneumonia, which has a mortality rate of 50 per cent in 72 hours.”
The Real Problem
Antibiotics have been a pillar of Western medicine for nearly a century. In a sad twist of irony, the very drug created to defeat disease has formed bacteria poised to run rampant through nations of the West. Yet mankind thinks it will dig itself out of this trouble once again. We have been through terrible times—even worse than this—before, man reasons.
Nowhere are these attitudes as common as in the West—specifically America and the United Kingdom. These two countries have enjoyed relative protection from disease epidemics, and it seems easy to chock up this disease-free time to democracy, to the marvels of modern science—due to “our own ingenuity.”
This cannot be further from the truth! The blessings the American and British peoples have long enjoyed have nothing to do with “ingenuity.” Unknown to most, the U.S. and Britain are descended from ancient Israel. But what does this have to do with prosperity or disease outbreaks?
America and Britain were blessed with prosperity simply for being descendants of the biblical patriarch Abraham. God promised his descendants blessings for his obedience. (David C. Pack explains this in great detail in his book America and Britain in Prophecy.)
In Leviticus 26, God makes plain the cause-and-effect relationship between obedience and disobedience. That is, as with any law—science or otherwise—laws will either keep you or break you. (Read Mr. Pack’s book The Ten Commandments – “Nailed to the Cross” or Required for Salvation? to learn more.)
The God of Abraham promised biblical-proportioned plagues for commandment-breaking: “But if you [Israel] will not hearken unto Me, and will not do all these commandments” (vs. 14), then…
• “I will even appoint over you terror, consumption [wasting lung disease] and the burning ague [fever]” (vs. 16).
• “I will bring seven times more plagues upon you according to your sins” (vs. 21).
• “I will send the pestilence among you” (vs. 25).
Sound harsh? Consider the blessings for obedience: “If you walk in My statutes, and keep My commandments, and do them” (vs. 3), then…
• “I will give you rain in due season” (vs. 4).
• “I will give you peace in the land…and I will rid evil beasts out of the land, neither shall the sword go through your land” (vs. 6).
• “I will have respect unto you, and make you fruitful, and multiply you” (vs. 9).
These blessings point to a Being who is far from “fiery” and vengeful. Instead, He is a God who wants to see people prosper and succeed.
In Exodus, God declares He is “the Lord that heals you” (15:26). This name is tied to obedience—doing what is right in the sight of God by keeping His Commandments and all His statutes.
This is not a God preached from the pulpits on Sunday. This is not a God who makes empty promises. Rather, He is the God who will hear heartfelt, contrite prayers of repentance—and heals those who “seek…first the kingdom of God, and His righteousness” (Matt. 6:33).
His promises for abundant health are outlined thoroughly in our booklets The Truth About Healing and God’s Principles of Healthful Living.
Other Related Items:
- The Ten Commandments – “Nailed to the Cross” or Required for Salvation?
- God’s Principles of Healthful Living
- America and Britain in Prophecy



